
What Are the 4 Types of Mental Health? A Practical Guide for Everyday Life

TLDR:
The four main types of mental health are emotional health, psychological health, social health, and behavioral health. Emotional health shapes how you experience and regulate feelings. Psychological health influences thinking patterns and resilience. Social health involves relationships and connection. Behavioral health reflects daily habits and coping behaviors. Together, these areas determine how people feel, function, and manage life’s challenges.
Introduction
Most people don’t search for “the four types of mental health” because they’re curious about definitions.
They search because something in their life feels harder than it used to.
Maybe emotions feel heavier. Maybe stress doesn’t fade the way it once did. Maybe relationships feel more draining. Maybe habits have shifted and sleep feels off. Or maybe everything looks fine on the outside, but inside things feel unsettled.
Mental health is often talked about like it’s one thing. In reality, it’s made up of several parts that work together every day. When one area starts to struggle, the others usually feel it too.
That’s where the idea of four main types of mental health comes from.
These types help explain how feelings, thoughts, relationships, and daily behaviors all shape well being. They aren’t labels or diagnoses. They’re ways of understanding what might be driving stress, exhaustion, anxiety, or emotional overload in real life.
In the sections ahead, we’ll walk through emotional mental health, psychological mental health, social mental health, and behavioral mental health, what each one means, how it shows up day to day, and why they matter together.
The Four Core Types of Mental Health
Mental health doesn’t exist in a single box.
It develops through several interconnected areas that shape how people experience emotions, process thoughts, build relationships, and manage daily life. These areas work together constantly. When one begins to struggle, the others often feel the impact.
That’s why many professionals describe mental health through four core types. Each one highlights a different part of well being, but none operates alone.
Understanding these types helps explain why stress can affect sleep, why emotional strain can change behavior, and why relationship problems can intensify anxiety or low mood.
Let’s begin with emotional mental health, the area most people recognize first when something starts to feel off.
Emotional Mental Health: How You Experience and Regulate Feelings
Emotional mental health reflects how you experience emotions and how you move through them day to day.
It involves noticing what you feel, understanding why those feelings show up, and regulating reactions when stress rises. Strong emotional health doesn’t mean life feels easy or positive all the time. It means emotions shift in ways that feel manageable instead of overwhelming.
When emotional mental health feels strong, people often:
• recognize emotions without judging themselves
• respond to stress without constant panic or shutdown
• recover more quickly after hard moments
• feel a full range of feelings without getting stuck in them
Strong emotional health allows people to feel sadness without sinking into despair, frustration without exploding, and stress without spiraling.
When emotional mental health feels strained, everyday life usually looks different.
People may experience:
• constant worry or irritability
• emotional exhaustion by the end of the day
• sudden mood swings
• numbness or feeling disconnected
• difficulty calming down after stress
Many people with strained emotional health still function outwardly. They go to work, care for family, and keep routines going. Inside, emotions feel heavier and harder to manage than they used to.
Emotional mental health matters because emotions guide how the body responds to life. When feelings stay in a constant state of tension, sleep suffers, concentration drops, relationships strain, and stress builds faster.
For example, someone may snap at loved ones over small things, replay worries late at night, or feel drained by situations that once felt manageable.
As emotional health improves, people often notice calmer reactions, clearer thinking, better sleep, and a greater sense of control over daily stress.
Psychological Mental Health: How Thoughts Shape Experience and Resilience
Psychological mental health focuses on how the mind processes life.
It involves thought patterns, beliefs about yourself and the world, problem solving, emotional insight, and the ability to adapt when things don’t go as planned. This area plays a major role in how people interpret stress, setbacks, and everyday challenges.
Strong psychological mental health doesn’t mean someone never worries or feels discouraged. It means the mind can stay flexible instead of getting stuck in cycles of fear, hopelessness, or self criticism.
When psychological mental health feels steady, people often:
• approach challenges with perspective instead of panic
• adapt when plans change
• recover after disappointment
• speak to themselves with fairness rather than harshness
• solve problems without feeling overwhelmed
Resilience grows from this flexibility. People bend under stress without breaking.
When psychological mental health feels strained, thought patterns often shift in ways that make life feel heavier.
Common signs include:
• constant overthinking or rumination
• assuming the worst will happen
• harsh inner self talk
• feeling helpless or stuck
• difficulty concentrating
Many people describe it as feeling trapped inside their own thoughts.
For example, a minor mistake at work may spiral into fears of failure. A difficult conversation may replay in the mind for days. A setback may feel like proof that nothing will improve.
Psychological mental health matters because thoughts influence emotions, behavior, and physical stress responses. When the mind stays locked in negative loops, anxiety rises, motivation drops, and exhaustion follows.
As psychological health improves, people often notice clearer thinking, improved confidence, better focus, and a stronger ability to handle life’s ups and downs without feeling overwhelmed.
Social Mental Health: How Connection and Relationships Support Well Being
Social mental health reflects how people connect with others and experience relationships.
It includes trust, communication, boundaries, support systems, and a sense of belonging. Humans are wired for connection. Healthy relationships help regulate stress, improve mood, and provide stability during difficult times.
Strong social mental health doesn’t mean having a large social circle. It means feeling supported, understood, and safe in meaningful relationships.
When social mental health feels strong, people often:
• communicate openly and respectfully
• feel comfortable asking for help
• trust others without constant fear of rejection
• maintain healthy boundaries
• feel connected rather than isolated
These connections act as emotional anchors during stressful moments.
When social mental health feels strained, life can feel much heavier.
People may experience:
• loneliness even when around others
• frequent relationship conflict
• withdrawal from friends or family
• fear of judgment or abandonment
• difficulty trusting people
Many people struggling socially still appear fine on the surface. Inside, they may feel disconnected, misunderstood, or emotionally alone.
Social mental health matters because relationships directly affect emotional stability and stress levels. Strong connections help buffer anxiety, sadness, and burnout. Poor connection often intensifies them.
For example, someone under work stress may cope well when supported by friends or family, but feel overwhelmed when isolated. Another person may struggle with mood simply because they feel unseen or unheard.
As social health improves, people often notice greater emotional balance, reduced stress, improved confidence, and a stronger sense of belonging.
Behavioral Mental Health: How Daily Habits Shape Well Being
Behavioral mental health focuses on what people do each day and how those actions affect emotional and psychological health.
It includes sleep patterns, eating habits, physical activity, substance use, work routines, and coping behaviors during stress. These everyday actions may seem small, but over time they strongly influence mood, energy, and mental clarity.
Strong behavioral mental health doesn’t require perfect habits. It involves patterns that generally support rest, balance, and recovery.
When behavioral mental health feels steady, people often:
• sleep fairly consistently
• eat regular meals
• stay somewhat active
• manage stress without relying on harmful coping behaviors
• keep routines that provide structure
These habits help the brain regulate emotions and handle daily pressure.
When behavioral mental health feels strained, routines often shift in ways that worsen stress.
Common signs include:
• chronic poor sleep or insomnia
• skipping meals or overeating
• withdrawing from activity
• relying on alcohol, substances, or excessive screen time to cope
• difficulty maintaining daily responsibilities
Many people notice these changes before they recognize emotional or psychological strain.
Behavioral mental health matters because the brain and body function as a system. Poor sleep increases anxiety. Unstable routines worsen mood. Unhealthy coping behaviors intensify emotional distress.
For example, someone feeling anxious may stay up late scrolling on their phone to distract themselves, which leads to exhaustion the next day, making anxiety worse. Over time, this cycle becomes hard to break.
As behavioral health improves, people often notice better energy, clearer thinking, more stable mood, and improved ability to manage stress.
Cognitive Mental Health: How Attention, Memory, and Thinking Skills Affect Daily Life
Cognitive mental health focuses on how the brain processes information.
It includes attention, memory, learning, problem solving, decision making, and mental clarity. This area shapes how well people concentrate at work, follow conversations, organize tasks, and respond to stress.
Strong cognitive mental health doesn’t mean perfect focus all the time. It means the brain can stay flexible, engaged, and clear enough to handle daily demands.
When cognitive mental health feels steady, people often:
• focus without constant distraction
• remember information more easily
• think clearly under pressure
• make decisions with confidence
• organize tasks without feeling overwhelmed
When cognitive mental health feels strained, everyday functioning becomes harder.
Common signs include:
• difficulty concentrating
• forgetfulness
• mental fog
• slowed thinking
• trouble completing tasks
• feeling easily overwhelmed by simple decisions
Many people describe it as their brain feeling tired or overloaded.
Cognitive strain often appears during periods of anxiety, depression, burnout, poor sleep, or chronic stress. The brain struggles to process information efficiently when emotional and physical systems remain under pressure.
For example, someone experiencing high stress may reread the same email multiple times without absorbing it. Another person with low mood may struggle to plan simple daily tasks.
Cognitive mental health matters because clear thinking supports emotional regulation, productivity, and confidence. When focus and memory suffer, frustration rises and stress builds faster.
As cognitive health improves, people often notice sharper focus, better organization, improved confidence, and a greater sense of control over daily responsibilities.
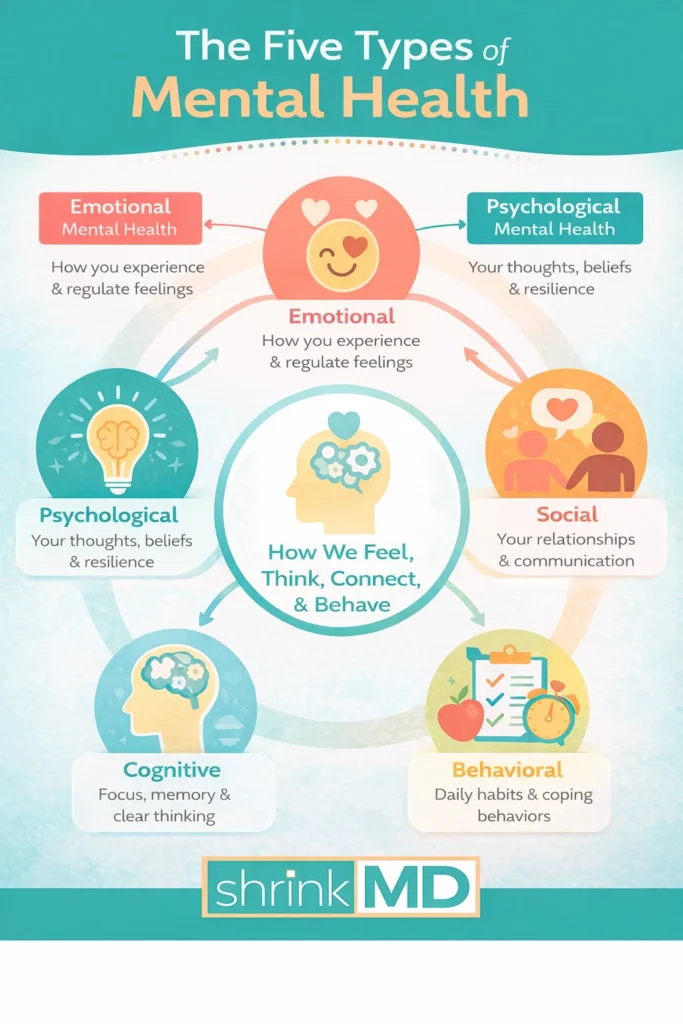
How These Types of Mental Health Work Together in Real Life
Mental health rarely affects just one area at a time.
Emotions, thoughts, relationships, habits, and cognitive focus constantly influence each other. When one area begins to struggle, the others often respond without you realizing it.
That’s why mental health can feel complicated and why simple solutions rarely work.
For example, ongoing stress may strain emotional health first. Anxiety rises and patience drops. That emotional tension then affects psychological health as negative thoughts loop faster. Concentration becomes harder as cognitive health feels foggy. Sleep suffers as behavioral patterns shift. Relationships may strain as social health feels harder to maintain.
All of this can start from one area but quickly spread across the system.
Another person may begin with poor sleep due to work pressure. Fatigue weakens focus and memory. Frustration grows emotionally. Motivation drops psychologically. Social withdrawal follows. Before long, life feels heavier than expected.
Mental health moves like a web, not a straight line.
This doesn’t mean something is wrong with you. It means your brain and body respond to stress as an interconnected system.
When care supports multiple areas at once, recovery often feels smoother and more lasting. Improving sleep can reduce anxiety. Strengthening relationships can improve mood. Learning coping skills can calm emotions. Addressing thought patterns can restore focus.
Real progress usually happens when emotional, psychological, social, behavioral, and cognitive health receive attention together.
That’s why mental health treatment often blends therapy, lifestyle changes, emotional skills, and sometimes medication. Each piece supports the others.
Understanding this interaction helps people feel less frustrated when healing takes time and more hopeful when small improvements start to create bigger change.
How the Four “P” Factors Help Explain Mental Health
When we talk about what shapes mental health, it helps to look at a flexible framework clinicians use every day in practice. The four “P” factors — predisposing, precipitating, perpetuating, and protective factors — offer a clear way to understand why struggles start, how they continue, and what supports recovery.
This framework isn’t a diagnostic list. It isn’t a set of labels. It’s a way of thinking that connects experiences, biology, stressors, and support so people can make sense of their mental health more deeply and honestly.
Predisposing Factors: The Setup
Predisposing factors are the background influences that make someone more vulnerable to emotional or mental strain. These can include:
• genetics or family history of mental health conditions
• long term stress exposure
• early life adversity
• temperament or personality traits
• medical conditions that affect mood or cognition
Predisposing factors don’t cause mental health challenges on their own. They simply influence how easily someone’s nervous system responds to life stress.
Precipitating Factors: What Triggers Struggles
Precipitating factors are the events or experiences that push someone toward distress.
These often include life changes or stressful experiences such as:
• loss or grief
• major transitions (work, relationships, relocation)
• trauma or significant setbacks
• chronic stress overload
These triggers help explain why symptoms can appear suddenly or feel more intense at certain times.
Perpetuating Factors: What Keeps Struggles Going
Perpetuating factors are the patterns that unintentionally maintain distress long after the original trigger has passed. These may include:
• disrupted sleep and poor routines
• withdrawing from social support
• avoidance behaviors
• negative thinking loops
• unhealthy coping habits
For example, someone might begin worrying intensely after a stressful event, but ongoing poor sleep and constant self-criticism keep the worry alive and make it harder to recover.
Understanding perpetuating factors helps people see how their daily habits and thought patterns influence emotional and psychological health.
Protective Factors: What Supports Resilience
Protective factors are the supports and strengths that help buffer stress and promote recovery. These can include:
• supportive relationships
• healthy routines and coping skills
• access to care and therapy
• physical health and sleep quality
• purposeful activities and community connection
Protective factors don’t prevent challenges entirely, but they help people bounce back faster and with more confidence.
Why the Four “P” Factors Matter
This framework shows that mental health doesn’t come from a single cause. It emerges from the interplay between biology, experience, stress, habits, and support systems.
Understanding the four P’s helps people and clinicians work together to:
• see patterns instead of blame
• target areas for practical change
• recognize early warning signs
• build strength in more than one area at a time
In everyday life, this means people can notice not just what they struggle with, but why it matters, and how they can support change that lasts.

Common Myths That Cause Confusion About Mental Health Types
Mental health often gets oversimplified online and in everyday conversations. These myths can make people misunderstand what they’re experiencing or delay getting support that could help.
Let’s clear up some of the most common ones.
Myth 1: Mental health types are fixed categories
Mental health doesn’t live in separate boxes. Emotional, psychological, social, behavioral, and cognitive health constantly interact. A struggle in one area usually affects the others. These types exist to explain patterns, not to label people permanently.
Myth 2: Emotions are the only part of mental health
Feelings matter, but mental health involves far more than mood. Thought patterns, relationships, habits, focus, sleep, and stress responses all shape well being. Someone can feel emotionally “okay” while still struggling mentally or behaviorally.
Myth 3: Social health doesn’t affect mental health much
Connection strongly influences mood, anxiety, and resilience. Isolation often worsens depression and stress. Supportive relationships help regulate emotions and protect mental well being. Social health plays a central role in recovery and stability.
Myth 4: Cognitive struggles mean someone isn’t trying hard enough
Difficulty focusing, remembering, or thinking clearly often comes from stress, anxiety, poor sleep, or low mood. These changes reflect how the brain responds to strain, not laziness or lack of effort.
Myth 5: Strong mental health means you never struggle
Healthy mental health doesn’t remove stress, sadness, or worry. It allows people to experience challenges without becoming overwhelmed or stuck in them. Everyone has hard days. Strength comes from recovery and flexibility, not perfection.
Myth 6: Habits don’t really impact mental health
Sleep, routines, substance use, and daily coping behaviors directly affect mood and focus. Poor habits often intensify anxiety and depression. Healthier routines frequently improve emotional stability.
Myth 7: Mental health problems always come from one cause
Most struggles develop from a mix of stress, biology, experiences, habits, and relationships. There’s rarely a single trigger. Understanding the full picture helps treatment work better.
How to Support Each Type of Mental Health in Everyday Life
Supporting mental health rarely comes from one big change.
Most lasting improvement grows from small, steady adjustments across emotional, mental, social, and daily life patterns. When people focus on only one area, progress often feels limited. When they support several areas together, the nervous system begins to settle and resilience builds naturally.
Mental health improves the same way physical health does. Consistent habits, healthy coping strategies, supportive relationships, and balanced thinking slowly strengthen the system over time.
The goal isn’t perfection. It’s creating enough stability that stress feels manageable instead of overwhelming.
Below are practical, realistic ways people can support each type of mental health in everyday life.
Supporting Emotional Mental Health
• pause and name emotions instead of pushing them away
• practice calming techniques like slow breathing or grounding
• give yourself space to feel without judgment
• reduce overload by setting limits when stress builds
Learning to notice and regulate feelings helps prevent emotional buildup from turning into anxiety or burnout.
Supporting Psychological Mental Health
• challenge harsh self talk with more balanced thinking
• break large problems into smaller steps
• reflect on stress triggers and responses
• practice flexibility when plans change
Developing healthier thought patterns improves resilience and emotional balance over time.
Supporting Social Mental Health
• reach out to trusted people regularly
• communicate needs clearly
• set boundaries that protect energy
• prioritize meaningful connection over quantity
Even one supportive relationship can significantly improve well being.
Supporting Behavioral Mental Health
• aim for consistent sleep and wake times
• eat regular balanced meals
• move your body in simple ways like walking
• limit reliance on alcohol or substances during stress
• build routines that create structure
Healthy habits stabilize mood and reduce emotional reactivity.
Supporting Cognitive Mental Health
• take short mental breaks during busy days
• focus on one task at a time
• protect sleep since clarity depends on rest
• reduce constant multitasking and screen overload
• write things down to ease mental load
Clearer thinking often improves when stress lowers and routines stabilize.

Frequently Asked Questions About the Types of Mental Health
What are the four main types of mental health?
The four commonly discussed types are emotional mental health, psychological mental health, social mental health, and behavioral mental health. Some frameworks also include cognitive mental health as a closely related fifth area. Together, these describe how people experience emotions, process thoughts, connect with others, and manage daily habits that influence well being.
Are these types official clinical categories?
No. These types are not formal diagnostic categories like those used in medical manuals. They are practical frameworks many mental health professionals use to explain how different parts of well being interact. They help people understand patterns in daily life and guide treatment in a more whole person way.
Can someone be strong in one type of mental health and struggle in another?
Yes, and this happens often. A person may have strong relationships and stable routines but still struggle with anxiety or low mood. Another may think clearly but feel emotionally overwhelmed. These areas influence each other, but they don’t always rise and fall at the same time.
Which type of mental health matters most?
None stands alone as most important. Emotional health often feels most noticeable because it affects mood day to day, but sleep, habits, relationships, and thought patterns strongly shape emotional stability. Mental health improves best when several areas receive support together.
How do these types connect to mental health disorders?
Struggles in these areas often show up as symptoms of conditions like anxiety, depression, burnout, trauma responses, and mood disorders. For example, emotional overwhelm, negative thinking loops, social withdrawal, poor sleep, and difficulty concentrating commonly occur together. A professional evaluation helps clarify how these patterns fit into a specific diagnosis and treatment plan.
What does emotional mental health actually involve?
Emotional mental health reflects how people experience, understand, and regulate feelings. It affects stress tolerance, mood stability, and recovery after hard moments. When emotional health improves, people often feel calmer, less reactive, and better able to handle daily pressures.
How is psychological mental health different from emotional health?
Psychological mental health focuses on thinking patterns, beliefs, problem solving, and mental flexibility. Emotional health relates to feelings themselves. For example, sadness is emotional, while thoughts like “nothing will ever get better” are psychological. The two constantly influence each other.
Why is social mental health so important?
Social mental health reflects connection, trust, communication, and support. Strong relationships help regulate stress and protect against anxiety and depression. Isolation and ongoing conflict often worsen emotional distress, even when other parts of life seem stable.
How do daily habits affect mental health?
Behavioral mental health includes sleep, eating, activity, substance use, and coping routines. These habits directly influence brain function and emotional balance. Poor sleep and inconsistent routines often intensify anxiety and low mood, while healthier patterns usually improve mental stability across the board.
What is cognitive mental health and why does “brain fog” happen?
Cognitive mental health involves focus, memory, decision making, and mental clarity. Brain fog often appears during periods of stress, anxiety, depression, burnout, or poor sleep. As emotional and physical strain decreases, cognitive clarity usually improves as well.
Can improving one area of mental health help the others?
Yes. These areas work as a system. Better sleep often reduces anxiety. Stronger relationships improve mood. Healthier thought patterns increase focus. Small improvements in one area frequently create positive changes across the others.
When should someone consider professional support?
Support can help when emotional distress lasts most days, thoughts feel stuck, relationships suffer, habits change significantly, or focus and energy drop noticeably. Early care often prevents symptoms from becoming more severe and helps people regain balance sooner.
A Gentle Closing Reflection
Mental health doesn’t look the same for everyone.
Some people struggle emotionally. Others feel stuck in their thoughts. Some feel disconnected from others. Some notice changes in sleep, focus, or daily routines long before they recognize emotional stress.
Most people experience a mix of these at different points in life.
That doesn’t mean something is wrong with you. It means your mind and body are responding to pressure, change, and experience in very human ways.
Understanding the different types of mental health helps people recognize what might be driving stress and where healing can begin. It reminds us that mental health isn’t weakness and it isn’t one dimensional. It’s a system that can become strained and also recover.
Support is common. Improvement is possible. And no one has to figure it out alone.
Some people choose to work with teams like shrinkMD when they want thoughtful psychiatric care that fits into real life.
Others begin with small changes, conversations, and awareness.
Every path toward feeling better is valid.
Five Key Takeaways
- Mental health includes emotional, psychological, social, behavioral, and cognitive well being that work together every day.
- Struggles in one area often affect the others, which is why mental health is not one dimensional.
- Emotions, thoughts, relationships, habits, and focus all shape how people feel and function in daily life.
- Small consistent changes across multiple areas often lead to the strongest improvements in mental health.
- Mental health challenges are common, understandable, and highly treatable with the right support.
Disclaimer
This article is for general educational purposes only. It does not provide medical advice and does not establish a doctor patient relationship. If you have concerns about your mental health or symptoms, please seek care from a qualified healthcare professional.
About the Author
You May Like
What Psychiatry Actually Does (and When It Helps)
TLDR:Psychiatry isn’t just about diagnoses or medication. It’s about understanding patterns over time, how the brain and body interact, and when symptoms need a broader medical lens. When used thoughtfully, psychiatry works best alongside therapy to support clarity, stability, and long-term well-being. Introduction Psychiatry is often one of the most

Dealing With Super Bowl Loss: Why It Hurts So Much and How to Recover Emotionally
TLDR:A Super Bowl loss can hit harder than expected because it carries months of anticipation, identity, and emotional investment. Reactions like anger, sadness, or replaying the game are normal responses to meaningful loss, not weakness. Most Super Bowl loss mental health reactions ease within a few days when emotions are

Telepsychiatry Is Changing Mental Health Care. Here’s the Part No One Explains.
TLDR:Telepsychiatry didn’t change mental health care because it’s convenient. It gained relevance because it solved real, long-standing barriers in access, continuity, and consistency. The clinical value comes from the timing and quality of care, not whether someone sits in the same room as their clinician. Introduction Telepsychiatry is no longer
